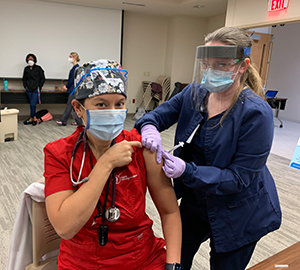
COVID-19 Vaccine Information
Frequently Asked Questions About the COVID-19 Vaccine
Who should receive the vaccine?
Who should not receive the vaccine?
Anyone who has had prior severe allergic reactions.
How will the vaccine be administered?
The vaccine will be administered to the arm as a two-shot injection 21-28 days apart.
What are the side effects?
If a patient is immunocompromised, will they mount a response?
The response may lower than a healthy individual, but a lower response is better than none.
How soon after being diagnosed with COVID 19 infection should a person receive the vaccine?
I've already had my first two shots and have been boosted. What about a fourth vaccine dose?
The CDC recommends that people with cancer get a FOURTH dose of the COVID-19 vaccine. Cancer patients face a greater risk of severe illness from COVID-19. Get vaccinated to reduce your risk of infection and complications. Cancer patients that are receiving treatment or have moderate to severe immunocompromising conditions are highly encouraged to get the FOURTH dose. Please talk with your physician about their recommendation.
Can a patient still get the vaccine if currently COVID-19 positive?
No. However, the testing is not routinely recommended prior to vaccination.
Do I still need to wear a mask after getting vaccinated?